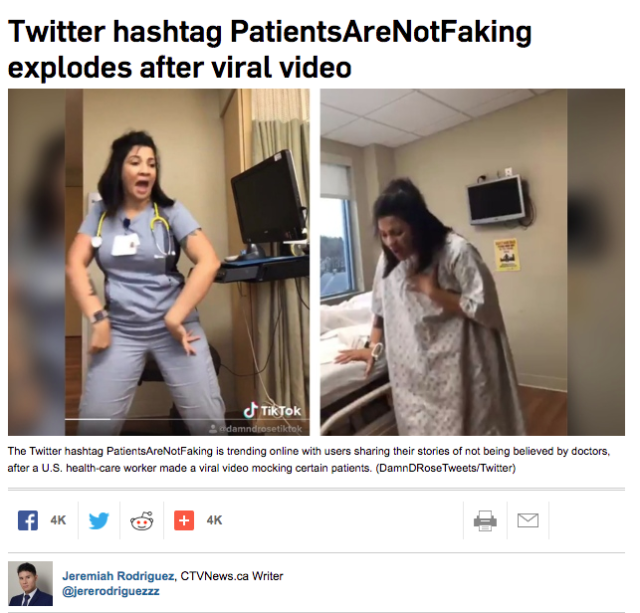
Kathleen Finlay Interviewed by CTV News on Disrespectful Viral Video
Patients and families, often already under enormous stress and worry, don’t need healthcare professionals mocking and disbelieving them. The woman in the video calls herself a nurse. My mother was a nurse. I know many nurses. This is no nurse in the true sense of that word. She has re-traumatized many patients and families, reminding […]