
LIFE RE-IMAGINED
Every year, 100,000 Canadians try to take their own lives. More than 4,000 die. Our system for preventing suicide is broken. We need to re-imagine our approach to this public health crisis, including providing faster access to intervention services, like a national 9-8-8 suicide prevention hotline. CTV Natonal News called it “three numbers that could make all the difference.” It could be the life ring that saves a son or daughter, a brother or sister, a wife, husband, or friend.
“It’s like being on the Titanic and people are in the water saying, ‘Please throw me a life ring. I’m drowning.’ You try to help as many people as you can, but there are so many of them. And some of them aren’t going to make it.”
— Former RCMP Constable Krista Carle in 2016. Krista died by suicide in 2018.
On Christmas Eve in 2019, famed Inuk singer Kelly Fraser died by suicide. She was 26. In the summer a year earlier, former RCMP Constable Krista Carle took her own life. Those two tragedies were extensively covered in the media. Most of the other thousands of suicides that occurred in 2018 and 2019 were not.
As Kathleen Finlay wrote in a recent op-ed in the Ottawa Citizen, in the past ten months alone, five University of Ottawa students have ended their lives by suicide. In the four-year period between 2013 and 2017, more than 1,000 youth took their own lives. One was only eight years old. During a single month in 2016, six young girls between the ages of 10 and 14 living in Northern Saskatchewan died by suicide.
- Suicide is the second leading cause of death for males between the ages of 15 and 24.
- LGBTQ youth are at significantly higher risk of suicidal thoughts and attempts at self-harm than their non-LGBTQ peers.
- First Nations populations have a suicide rate three times higher than the non-Indigenous population.
- Some reports have placed the suicide rate among Inuit in Nunatsiavut at 25 times the national rate.
- If Nunavut were a country, it would rank number one in the world for male suicide.
- Law enforcement officers are more likely than members of the general population to engage in suicidal behaviour, and they are more likely to die by suicide than they are in the line of duty.
- Former Canadian soldiers are at higher risk of suicide than the general population. Male veterans who died before the age of 25 were 2.4 times more likely to have died by suicide than their counterparts in the general population.
 These figures don’t begin to count the toll suicide takes among surviving family members and friends,who can face years tormented by feelings of guilt and regret. Each person who dies by suicide leaves behind as many as 10 survivors who are deeply affected by their loss. The Washington-based Centers for Disease Control estimates that for every person who dies by suicide, another 280 have considered ending their lives.
These figures don’t begin to count the toll suicide takes among surviving family members and friends,who can face years tormented by feelings of guilt and regret. Each person who dies by suicide leaves behind as many as 10 survivors who are deeply affected by their loss. The Washington-based Centers for Disease Control estimates that for every person who dies by suicide, another 280 have considered ending their lives.
Research has also shown that gender-based violence places victims at higher risk of suicide than the rest of the population. This risk is magnified when victims are blamed or punished after they come forward, or when they are subjected to institutional betrayal. A victim of former Canadian Senator Don Meredith’s sexual abuse reported that she had considered suicide, according to the findings of the Senate ethics commissioner. Those with PTSD are also known to be at high risk. Kelly Fraser and Krista Carle each struggled with PTSD.
During consideration of amendments to the federal government’s anti-harassment legislation (Bill C-65) in 2018, Kathleen Finlay made formal submissions regarding the risks posed to victims of gender-based violence and sexual harassment, including suicide.
Every death by suicide was a cry for help not heard, or not heeded, or not acted on. We will not be successful in ending the epidemic that is overtaking parts of our society until we end the factors that contribute to it, and make life-sustaining interventions easier and faster for those in a state of emotional trauma
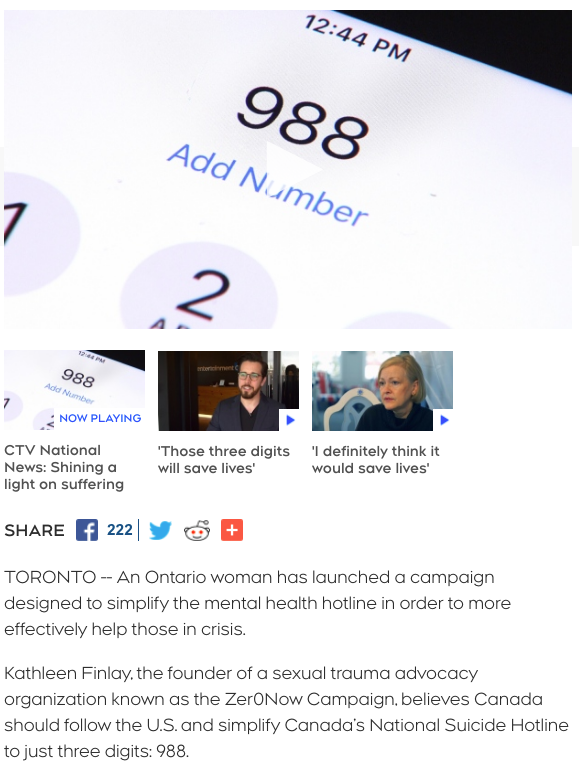
It is against this backdrop that Kathleen Finlay, founder of the The ZeroNow Campaign to combat sexual trauma, is campaigning for a life-saving innovation in suicide prevention. It’s a new, easy-to-remember, three-digit phone number, 9-8-8, for a national suicide prevention crisis line. It’s being called the 9-1-1 for mental health emergencies, and it’s currently being rolled out in the United States. Profiling Kathleen’s campaign, CTV National News has described 9-8-8 as “three numbers that could make all the difference.”
In Canada, tackling the crisis of suicide has clearly not yet garnered the political support needed for progress to be made. During the 2019 federal party leaders’ debates, for instance, the word “suicide” was not mentioned even once. Similar absence of any reference to suicide leaps out from the mandate letter for the federal minister of health, which was issued following the 2019 federal election.
Efforts by mental health advocates over many years to persuade the Canadian government to adopt and implement a national action plan to combat suicide have proven unavailing. But the evidence is clear that too many people are slipping through the current suicide prevention safety net.
It is a very different situation in the United States, where replacement of the current 11-digit toll-free national suicide hotline number by the new, faster 9-8-8 dialing code is well underway. The innovation came about after the National Suicide Hotline Improvement Act was signed into law in 2018. The Act required “the Federal Communications Commission to study the feasibility of designating a simple, easy-to-remember dialing code to be used for a national suicide prevention and mental health crisis hotline system.”
 The legislation’s co-author, (now retired) Senator Orrin Hatch, said on passage of the bill in the House of Representatives:
The legislation’s co-author, (now retired) Senator Orrin Hatch, said on passage of the bill in the House of Representatives:
I believe that by making the National Suicide Prevention Lifeline system more user-friendly and accessible, we can save thousands of lives by helping people find the help they need when they need it most. Every minute we wait, we leave helpless hundreds of Americans who are struggling with suicidal thoughts. There are literally lives on the line here—and leaving them on hold is not an option.
The bill, which passed unanimously in the Senate, missed unanimous support in the House by just one vote. Such bipartisan consensus in America is rare, and it underscores the sense of urgency surrounding suicide as a public health crisis in the U.S.
Hatch said he began the effort because he believed the existing National Suicide Prevention Lifeline system and Veterans Crisis Line were “in desperate need of reform.” The current lifeline number “is not an intuitive or easy number to remember — particularly for those experiencing a mental health emergency,” he argued.
As a result of lawmakers actually leading in the war against suicide, in 2019 the U.S. Federal Communications Commission recommended that 9-8-8 replace the existing 11-digit toll-free number for the national suicide prevention hotline. The choice came about after extensive consultations with mental health advocates and healthcare professionals, which included a lengthy analysis of various three-digit alternatives, such as 611, 211, and an expansion of existing 911 services. In the end, the new and never before used numeric combination of 9-8-8 was the overwhelming choice. 
Think about where we’d be today if, instead of dialing 9-1-1, we had to use the phone book or search Google to find a seven- or 11-digit telephone number for first responders, like police, ambulance and fire. What if it was a different number for every city, community and province? Think of 9-8-8 as the mental health equivalent of 9-1-1.
Renowned Columbia University psychologist Madelyn Gould, PhD, an expert in suicide prevention, recently told National Public Radio in the U.S., “People can have a cognitive shutdown or blank, as any of us do, when we can’t remember things during times of extreme stress.” Having a three-digit hotline, she says, will “facilitate people’s access to care at times when they are in dire need.”
The shift to the 9-8-8 hotline has the full backing of the U.S. mental health community. As Melba Vasquez, PhD, former president of the American Psychological Association told Kathleen Finlay in an exclusive interview, 9-8-8 will “absolutely” save lives. She said it will also help to reduce the stigma associated with reaching out in a time of mental health crisis “by normalizing the occurrence of need.”
The evidence is overwhelming that 9-8-8 will work in getting help faster to those struggling in a time of emotional crisis, and because of that, it will save lives. But, in Canada, the idea of moving to a three-digit hotline number that would be easier to remember, faster to dial and quicker to deliver life-saving help than the current 11-digit hotline number is nowhere on the radar of federal politicians. As Kathleen Finlay told CTV National News, “I’ve been knocking on the social media doors of the Prime Minister, cabinet ministers, all the federal party leaders, MPs and senators. I did it before the election. I did it during the election. I did it after the election. Not a single person has responded. That’s really disheartening.” Interviewed by The Hill Times, Kathleen said “silence is never the right response when suicide is the subject.”
 The CTV National News segment about this innovation in mental health care kicked off news coverage of Bell Media’s annual Let’s Talk campaign. After the story aired, families of loved ones lost to suicide began to reach out to Kathleen to show their support for her campaign to bring 9-8-8 to Canada. In an op-ed running in the Ottawa Citizen, Kathleen noted:
The CTV National News segment about this innovation in mental health care kicked off news coverage of Bell Media’s annual Let’s Talk campaign. After the story aired, families of loved ones lost to suicide began to reach out to Kathleen to show their support for her campaign to bring 9-8-8 to Canada. In an op-ed running in the Ottawa Citizen, Kathleen noted:
Since I began my campaign to bring 9-8-8 to Canada, I‘ve talked with dozens of family members who lost loved ones to suicide. I am one myself. We all see the life-saving potential of 9-8-8. What we can’t understand is why Canada isn’t moving to adopt it as quickly as possible. As one still-grieving mother told me, if it saves just one life, it will be worth it.
It is baffling that an idea so enthusiastically embraced by U.S. politicians would be greeted with a huge yawn by Canadian lawmakers. It is, after all, not an additional or new resource that is being recommended, but a faster and easier pathway to connect with existing counseling services.
Right now, Canada has a toll free suicide prevention hotline staffed by well-trained and dedicated volunteers. But the 11-digit phone number is just as long and hard to recall as its U.S. counterpart. 
Complicating access to quick help even further, there are many online resources listed under “suicide prevention” (several of which receive funding from federal and provincial governments) that don’t even publish or display the national hotline number. Instead, they require visitors to scroll through lists of dozens of local crisis centres, many of which don’t operate on a 24/7 basis. One suggests Ontario residents in crisis call 211. The 211 website says it offers answers for those inquiring about services such as employment and training, housing, and other issues in addition to mental health. Callers have to navigate a menu, listen to a request that they complete a survey at the end of the call, and then wait for several minutes during a musical interlude for someone to respond. It’s too slow, and it’s definitely not a suicide prevention hotline.
When the FCC looked at three-digit numbers, it strongly rejected the use of 211 codes in the U.S., which are similar to those in Canada.
A person in crisis who is having suicidal thoughts needs to be seen as an urgent candidate for a life saved. Seconds count. They should not be left to make their way through a baffling maze when trying to get the help they want. Or face delays because of multiple layers of access, menus and re-connection steps.
A short, easy-to-remember 9-8-8 hotline number can change that.
Setting 988 for suicide prevention/mental health will save lives. My gratitude to forward-thinking elected officials like @RepChrisStewart and @sethmoulton, agencies like @samhsagov and @DeptVetAffairs, and organizations like @NationalCouncil and @TrevorProject for their support. https://t.co/v9uFJM2VHq
— Ajit Pai (@AjitPaiFCC) December 12, 2019
nbsp;
Of course, tackling this growing public health crisis in Canada needs more than 9-8-8. Wider understanding of the importance of trauma-informed principles and better awareness of suicide risk indicators need to become integrated into the core practices of all organizations, from education and social services to law enforcement and the courts. A willingness on the part of institutions and people in positions of trust to make greater effort to avoid inflicting harm is part of the solution as well. Greater emphasis on the healing principles of compassion and kindness, which are templates for civil and respectful social interaction, are also key to fighting the sense of despair and hopelessness that is often a precursor to suicidal thought and actions. Canada is the only G7 nation that does not have an actual suicide prevention strategy, even though they have been shown to work. For more than three decades, suicide prevention advocates have called for such a strategy.
Above all, in a time of unprecedented emotional distress, increasing deaths of despair, overdoses and attempts at suicide magnified by the coronavirus pandemic, we need a national soul-searching to identify and address the social and economic determinants of mental health crisis and suicide. And we need those most affected —the current and potential consumers of the mental health services and their families— to be a much more visible and heeded part of that conversation.
We need a national action plan that recognizes and addresses these high-risk connections. We also need to make prevention methods more accessible, starting with the three-digit 988 hotline system that is being deployed in the U.S. Time for action is NOW. Please RT to save lives!
— Kathleen Finlay | 🇨🇦🇺🇸🇬🇧 (@ZeroHarmNow) January 1, 2020
@CanadianPM @AndrewScheer @theJagmeetSingh @yfblanchet @ElizabethMay @Carolyn_Bennett @PattyHajdu @MaryamMonsef @MarcMillerVM@BardishKW @Puglaas @CTV_AvisFavaro @theresaboyle @picardonhealth @TheHillTimes @cspyyc https://t.co/EJpjdXnLfe pic.twitter.com/pzlEYcGcI9
— Kathleen Finlay | 🇨🇦🇺🇸🇬🇧 (@ZeroHarmNow) January 1, 2020
The Zer0Now Campaign and Protection.Healthcare are calling for a federal national strategy on suicide prevention with an emphasis on bringing new thinking and fresh ideas to the table. If we are serious about addressing the soul crushing crisis of suicide that is taking so many lives, we need to re-imagine our approach to meeting the needs of those most affected, including providing a faster life line like a 9-8-8 hotline.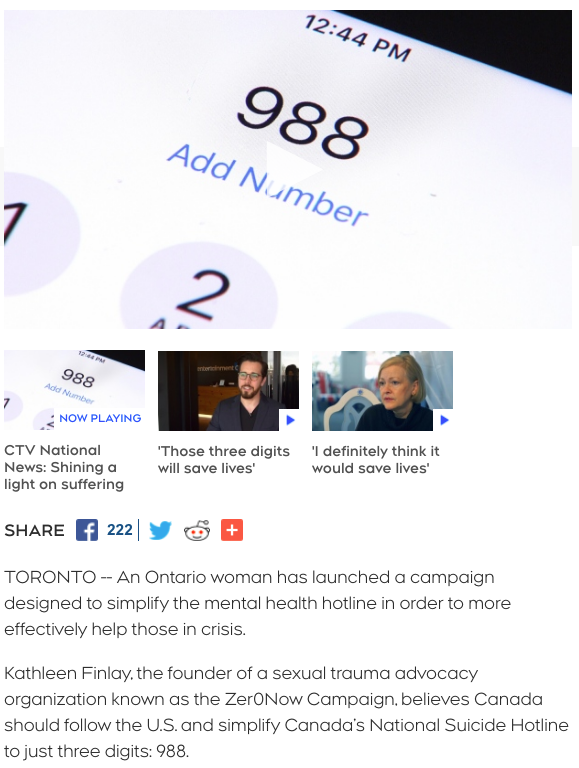
Your thoughts, ideas and support can make such a difference. You can share them here.
REALATED
The 988 Campaign for Canada
A Roadmap for the Government to Act Against Gender-Based Violence
Can Three Numbers Stem the Tide of American Suicides?


